| Osmotic demyelination syndrome | |
|---|---|
| Other names | Central pontine demyelination, central pontine myelinolysis, extrapontine myelinolysis |
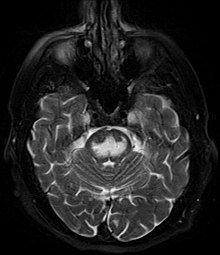 | |
| MRI image showing hyperintensity in the pons with sparing of the peripheral fibers, in a person with alcoholism and an initial serum Na of 101 who was treated with hypertonic saline, and developed quadriplegia, trouble talking, and altered mental status. | |
| Specialty | Neurology |
| Symptoms | Difficulty swallowing, difficulty speaking, movement disorders, decreased level of consciousness, paralysis[1] |
| Complications | Seizures, locked in syndrome[1] |
| Usual onset | One day to two weeks of a trigger[1] |
| Causes | Complication of rapid correction of low sodium[1] |
| Risk factors | Alcoholism, malnutrition, liver transplantation, kidney failure[1] |
| Diagnostic method | Suspected based on symptoms, confirmed by MRI[1] |
| Differential diagnosis | Hypertensive encephalopathy, multiple sclerosis, brainstem stroke, pontine neoplasms, CNS lymphoma, progressive multifocal leukoencephalopathy[2] |
| Prevention | Correct sodium at a rate of less than 0.5 mmol/L per hour[1] |
| Treatment | Supportive care |
| Frequency | Rare[1] |
Osmotic demyelination syndrome, previously known as central pontine myelinolysis, is damage to certain regions of the brain following rapid correction of electrolyte disorders.[2] Symptoms may include difficulty swallowing, difficulty speaking, movement disorders, decreased level of consciousness, and paralysis.[1] Other complications may include seizures and locked in syndrome.[1] Onset is within a day to two weeks of a trigger.[1]
It most commonly occurs as a complication of low sodium, particularly severely low sodium and its correction by more than 12 mmol/L in a day.[1] Other potential causes include low potassium, high sodium, low phosphate, liver transplantation, high blood sugar, and kidney failure.[1] Risk factors include alcoholism and malnutrition.[1] The underlying mechanism involves a rapid rise in serum tonicity leading to demyelination of white matter.[2] While the initial cases described the pons being affected, other areas of the brain have also found to be involved.[1] Diagnosis is suspected based on symptoms and confirmed by MRI.[1]
Prevention is by correcting low sodium at a rate of less than 0.5 mmol/L per hour.[1] Once the condition has developed there is no specific treatment, though immunotherapy and vaptans may be tried.[1] Poor outcomes occur in a third to half of those effected.[1] The risk of death is 10 to 60%.[1]
Osmotic demyelination syndrome is rare in the general population, though may affect up to 30% of at risk groups.[1] It most commonly occurs in those between the age of 30 and 50.[1] Males are more commonly affected than females.[1] It was first described by Adams in 1959.[1][3]
References
edit- ^ a b c d e f g h i j k l m n o p q r s t u v w x Lambeck, J; Hieber, M; Dreßing, A; Niesen, WD (2 September 2019). "Central Pontine Myelinosis and Osmotic Demyelination Syndrome". Deutsches Arzteblatt international. 116 (35–36): 600–606. doi:10.3238/arztebl.2019.0600. PMID 31587708.
- ^ a b c Danyalian, A; Heller, D (January 2022). "Central Pontine Myelinolysis". PMID 31869161.
{{cite journal}}: Cite journal requires|journal=(help) - ^ Adams, Raymond D. (1 February 1959). "Central Pontine Myelinolysis: A Hitherto Undescribed Disease Occurring in Alcoholic and Malnourished Patients". A.M.A. Archives of Neurology & Psychiatry. 81 (2): 154. doi:10.1001/archneurpsyc.1959.02340140020004.